Published By BHF | March 30, 2026
By: Tatumwa Desmond Benjamin
A life‑saving procedure marks a new chapter for women’s health in Busoga
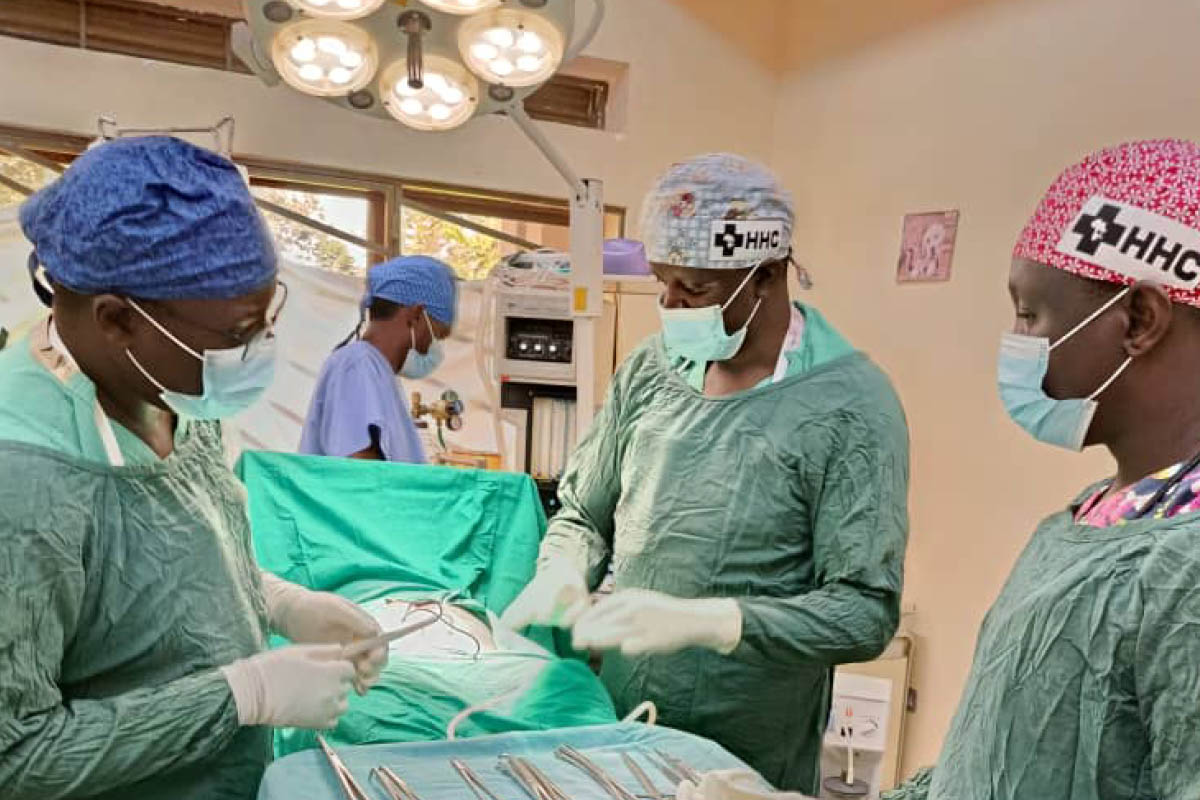
On 30 March 2026, a surgical team at HHC, led by Dr. Musana Othiniel (gyne‑oncologist) and Dr. Isaac Mubezi (general surgeon), performed the hospital’s first radical hysterectomy, a landmark achievement for the Busoga region. The patient had early‑stage cervical cancer (FIGO stage 1B). Radical hysterectomy is a complex operation that removes the uterus, cervix, upper vagina and nearby lymph nodes to eliminate cancerous tissue and provide the best chance of cure. By carrying out this procedure locally, HHC has shown that life‑saving oncology surgery can be delivered in the region with the right trained personel and resources rather than having women to travel to distant centres.
Why it matters
Cervical cancer is a major health burden in Uganda. According to the Uganda National Cervical Cancer Prevention and Control Strategic Plan (2018 – 2023), cervical cancer has the highest incidence among Ugandan women; the age‑standardised incidence and mortality rates are 44.4 and 27.4 per 100,000 women, respectively. The same report notes that approximately 3,915 women are diagnosed each year and about 2,275 die, and that over 80 % of patients present at an advanced stage, when survival is minimal. Globally, cervical cancer remains the fourth most frequently diagnosed cancer and fourth leading cause of cancer death among women, with about 604,000 new cases and 342,000 deaths worldwide in 2020. Almost all of the top 20 countries with the highest burden are in sub‑Saharan Africa, and limited access to prevention, screening and treatment contributes to 90 % of deaths.
Early detection dramatically improves outcomes. For invasive cervical cancer caught at an early stage, the 5‑year relative survival rate is about 92 %. A Tanzanian study of women with early‑stage cervical cancer treated with radical hysterectomy reported a 3‑year overall survival rate of 96.5 % and disease‑free survival of 79.1 %. These figures show that radical hysterectomy, when performed for well‑selected stage 1 patients, can be curative and offer excellent prospects for long‑term survival.
The Busoga breakthrough
Until now, women in Busoga who required a radical hysterectomy have to be referred to national centres, often facing long delays and prohibitive costs. HHC’s first successful radical hysterectomy demonstrates that the necessary skills and infrastructure are now available locally. Dr. Musana and Dr Mubezi’s collaboration brings together specialist oncologic and general surgical expertise, ensuring that the operation adheres to international standards of care. Their team’s achievement represents not only a surgical milestone but also an important message: with commitment and training, high‑quality cancer care can be decentralised to regional hospitals.
The surgery was performed on a woman with stage 1B cervical cancer, for which radical hysterectomy is an established treatment. As the procedure removes the uterus and cervix entirely, patients lose fertility, but the operation can provide a cure and prevent the need for chemoradiation. To reduce such difficult choices in the future, HHC will collaborate with Busoga Health Forum to launch community outreach for early cervical cancer screening and HPV vaccination. Screening allows detection of pre‑cancerous lesions that can be treated before invasive cancer develops, and vaccination prevents infection with high‑risk human papillomavirus, the virus that causes most cervical cancers.
Looking ahead
HHC’s inaugural radical hysterectomy sends a powerful message across Busoga:
- Early diagnosis saves lives. Most Ugandan women still present with advanced disease. By promoting screen‑and‑treat strategies and encouraging women to attend routine screening, HHC hopes to catch cervical cancer at pre‑cancerous or early stages when treatment is most effective.
- Investing in local surgical capacity pays off. HHC’s success shows that regional hospitals can develop the expertise to perform complex oncologic surgeries. This reduces travel burdens and brings care closer to patients.
- Collaboration is key. The partnership between gyne‑oncology and general surgery at HHC illustrates how pooling skills can overcome resource limitations. Continued training, mentorship and investment will be needed to sustain and expand this programme.
Cervical cancer need not be a death sentence. With early screening, HPV vaccination and access to curative surgery, thousands of women’s lives can be saved. The Busoga community should celebrate this milestone and support initiatives that ensure no woman is denied timely care. HHC’s first radical hysterectomy is more than a surgical achievement – it is a commitment to a future where cervical cancer is detected early, treated effectively and ultimately eliminated.




